Mechanical Ventilation
What is ventilation?
A ventilator helps an individual breath and it is one of the most common interventions in an ICU. Patients who find it difficult or impossible to breathe are assisted by a ventilator that can perform the task for them thereby allowing their bodies to rest. Ventilation delivers oxygen to the body, expels CO2, and generally eases the burden of breathing. One must be aware though, that a ventilator does not cure an illness it merely sustains life of the patient while doctors determine the cause of the problem and devise the right treatment.
Non-invasive Ventilation
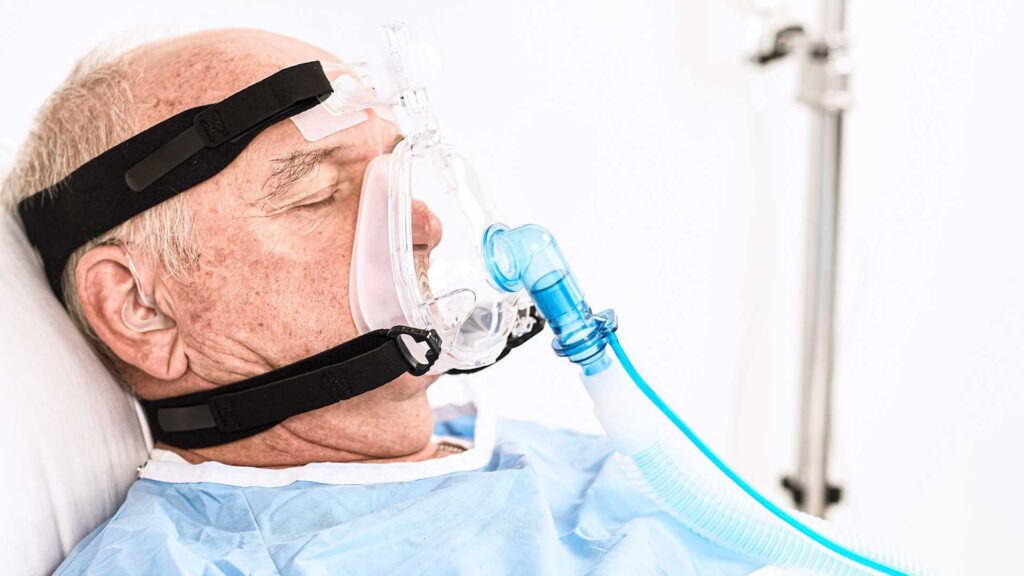
Noninvasive ventilation (NIV) is a term that refers to the use of external breathing support. NIV provides oxygen through a mask over the patient’s face or nose. In comparison, invasive ventilation is delivered via tracheostomy or endotracheal tubes. While invasive ventilation can be a lifesaving technique, complications can occur, including injury to the trachea and larynx, speech and swallowing disabilities, ventilator-associated pneumonia, and more. Noninvasive methods may be just as — or even more — effective and present less risk when used in appropriately chosen patients.
When does one require ventilation
A ventilator is required in case of respiratory failure. CO2 levels in the body may be rising or oxygen level in the blood may be very low. A compromised airway or lung function due to an underlying medical condition could also warrant the use of a ventilator to make breathing easier for the patient.
- To get oxygen into the lungs and body
- To help the lungs get rid of carbon dioxide
- To ease the work of breathing—Some people can breathe but it is very hard. They feel short of breath and uncomfortable.
- To breathe for a patient who is not breathing because of brain damage or injury (like a coma) or high spinal cord injury or very weak muscles. If a person has had a serious injury or illness that causes breathing efforts to stop, a ventilator can be used to help the lungs breathe until the person recovers.
-
Oxygen Concentrator Rental- DeVilbiss-5LPM
₹6,000.00 +GST Extra -
Oxygen Concentrator Rental – Phillips 5 LPM
₹6,000.00 +GST Extra -
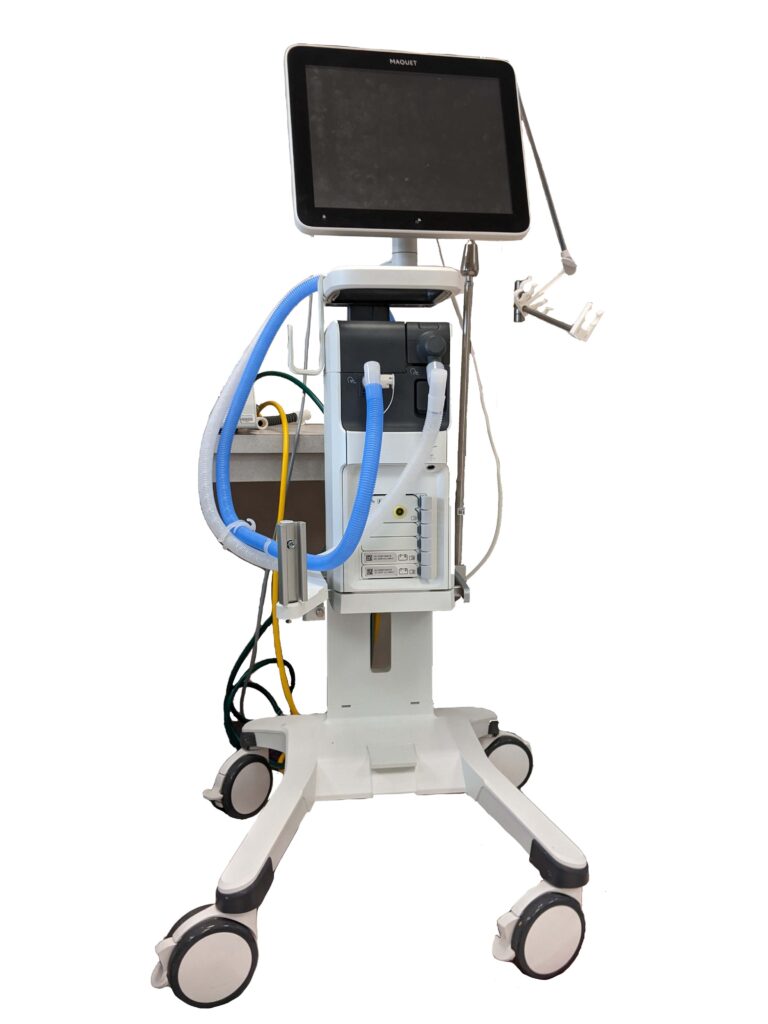
Ventilator Machine Rentals – Luisa Ventilators
₹3,000.00 +GST Extra




